Burn Definition
“What is skin grafting and flap surgery? A detailed question and answers guide”
It is a type of coagulative necrosis caused by heat, transferred from the source to the body. Frostbite, which occurs in cold countries, is also a coagulative necrosis, but it is caused by extreme degrees of cold. Hence, it is not a burn. Scald is a burn caused by moist heat (steam). Burns never occur at temperatures less than 44° C.
Burns Types
- Thermal: Flame burns and scald burns
- Electrical
- Chemical.
Read And Learn More: Clinical Medicine And Surgery Notes

“Understanding skin grafting and flap surgery through FAQs: Indications, techniques, and outcomes explained”
Pathophysiology Of Burns Shock
Although the exact mechanism of the postburn microvascular changes and hypovolaemia leading to low cardiac output and poor tissue perfusion has not been determined, the following various mechanisms have been proposed.
- Increased capillary permeability leads to fluid and protein leakage from the intravascular space.
- Decreased plasma oncotic pressure due to hypo-proteinaemia resulting from loss of protein from the intravascular space.
- Increased capillary hydrostatic pressure due to vasoconstriction or partial blockage of vessels with an aggregate of cells and platelets.
- Reduced clearance of fluid and protein from the interstitial space by lymphatic ducts due to blockage with platelet aggregates and fibrin clots.
- Intracellular fluid accumulation due to impaired cell membrane function.
- Increase osmotic pressure in burned tissue leads to further fluid accumulation.
- Increased evaporative water loss
- Depressed myocardial function
Chemical mediators released from the site of injury are responsible for the development of typical inflammatory responses. This results in rapid and dramatic edema formation.
- The activated complement cascade system facilitates the liberation of various permeability factors such as histamine, prostaglandins (PGF-1, PGF-2, PGF-2α), and thromboxane.
- Macromolecular leakage into burned areas, catabolism, and reduced immunoglobulin synthesis result in a decreased concentration of all individual immunoglobulin levels and triggering of the complement cascade.
Inhalation injury: Glottic edema, necrotizing bronchitis, and pneumonia are the dangerous events that follow an inhalation injury.
“How does skin grafting differ from flap surgery? FAQ answered”
Management Of Burns Patients
First aid: A cold water bath should be given immediately. This takes away the heat and
- stabilizes mast cells, thus decreasing the release of histamine, thereby reducing edema.
- Careful history, and duration since the time of injury with heat source should be recorded.
- Hospitalization and admission in the burns ward with air conditioning facility.
- Assessment of depth of burns
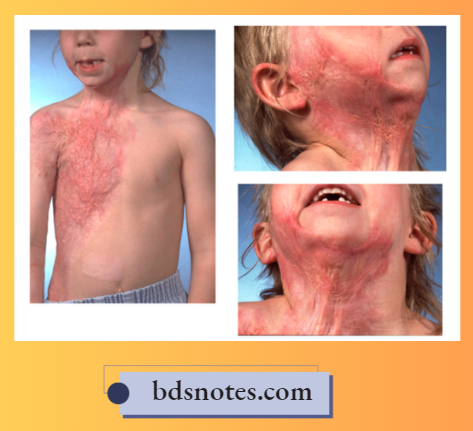
- Partial Thickness Burns: Here, Superficial Layers Of The Skin Are Destroyed. Epidermis And the Variable Portion Of Dermis Is Involved. Since The Nerve Endings Are Exposed, It Causes a Severe Degree Of Pain.
- Full thickness burns: Involvement of the full thickness of dermis with epidermis. Since the nerves are destroyed, it is less painful.
- Assessment of the extent of burns in terms of body surface area (BSA): It is calculated by a RULE OF 9 – RULE OF WALLACE
- Burns of head and neck: 9%
- Burns of upper limbs: 9 × 2 = 18%
- Burns of anterior trunk = 18%
- Burns of posterior trunk = 18%
- Burns of the lower limbs: 18 × 2 = 36% (front and back of each limb is 9%)
- Burns of external genitalia: 1%
- Temperature, pulse, respiration, and blood pressure have to be monitored and maintained.
- An indwelling urinary catheter (Foley’s catheter) is introduced, and a strict intake and output chart has to be maintained.
- A Ryle’s tube is passed. Burns patients can develop “acute stress ulcers” called acute peptic ulcers or Curling ulcers. Hence, to prevent bleeding, a cold stomach wash is given through Ryle’s tube, and antacids and H2 receptor blockers such as ranitidine 150 mg twice a day are given.
- Replacement of fluid volume
“Importance of studying skin grafting and flap surgery for medical students: Questions explained”
1. Muir and Barclay formula.
\(1 \text { ration }=\frac{\% \text { of burns } \times \text { body weight }}{2}\)3 rations in 12 hours, 2 rations in the next 12 hours, and 1 ration in the next 12 hours.
Example: 40% burns patients weighing 60 kg.
\(1 \text { ration }=\frac{40 \times 60}{2}=1200 \mathrm{ml}\)1st 12 hours: 3600 ml fluid
2nd 12 hours: 2400 ml fluid
3rd 12 hours: 1200 ml fluid
- The best replacement solution is plasma. For fear of transfusion reactions, a crystalloid such as Ringer’s lactate can be used.
- In any patient with burns above 20%, packed cells may be given in the 2nd ration (after 12 hours).
- After 36 hours, depending upon the urinary output and depending on the requirements of the body, about 2–3 liters of fluid are given in 24 hours.

“Common challenges in mastering skin grafting and flap surgery notes effectively: FAQs provided”
2. Parkland’s formula: 4 ml/ % /kg in the first 24 hours.
- 1/2: In 1st 8 hours
- 1/4: Next 8 hours each.
- 3. Modified Brooke’s formula:
- 1st 24 hours: 2 ml/% of burns/kg (deficit) + maintenance (2500 ml)
- 2nd 24 hours: 50% of the deficit in 1st 24 hours + maintenance (2500 ml in adults).
Rate of administration: 50% in the first 8 hours after injury and 50% in the next 16 hours.
10. Broad-spectrum antibiotics are given against gram +ve, gram −ve, and anaerobic organisms.
- To treat septic shock, higher antibiotics such as cephalosporins have to be given.
- Narcotic analgesics like injection morphine 10–12 mg IM or injection pethidine 60–75 mg IM is given to relieve the pain. (If the veins are not visible, a “cut down” needs to be done, so that the infusion cannula can be maintained for a long time.)
Treatment of burn wound
Clean the wound with antiseptic agents like Savlon, iodine, etc.
- Open method: Exposure line of management: If facilities available are good, with a fumigated ward, the wound can be left open to the atmosphere after applying Silver Sulfadiazine cream.
- Closed method: Alternately, after applying silver sulfadiazine, 1% silver nitrate, and mefenide cotton rolls are applied, over which a bandage is applied. This is called the closed method. The advantages of the closed method are less pain, reduced infection and sores, and better medication.
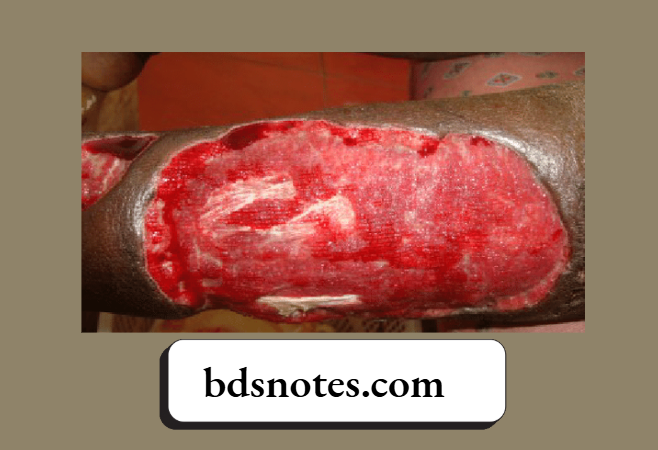
- Tangential excision followed by grafting is done after about 48–72 hours, in which the burn wound is excised tangentially till fresh bleeding occurs. This is followed by skin grafting. Skin is taken from the rest of the normal area, or can be obtained from the skin bank. A mesh expander and cell culture are also used.
“Why is proper technique critical for successful skin grafting? Answered”
Advantages of tangential excision
- It prevents secondary infection and septicemia.
- Decreases the hospital stay (2–5 weeks is the usual time taken for eschar of 3° burn to separate. This is cut short by tangential excision).
- Decrease of the incidence of contractures and hypertrophic scar.
- The cost of the treatment is reduced.
Causes of death in burns patients
- Uncontrolled hypovolemic shock (Refractory hypovolemia).
- Choking, and suffocation due to respiratory burns, especially burns of the head and neck.
- Septicaemic shock is the most common cause of death.
Prognosis
It depends upon several factors, the most important being the percentage of burns and the facilities of treatment.


“Factors influencing success with skin grafting and flap surgery studies: Q&A”
Factors Affecting Outcome
- Extremes of age
- Depth of burns
- Inhalation of noxious fumes
- Cardiopulmonary disease
Free Skin Grafting
Skin grafting is the most common method of achieving wound cover.
Free Skin Grafting Types
- Split skin graft (SSG – Thiersch graft)
- Also called a partial-thickness graft
- Consists of the epidermis and a variable portion of the dermis.
- Split skin graft is usually harvested using Humby’s knife. Drum Dermatome or power dermatome may also be used.
- The preferred donor area is the thigh.
- Full-thickness graft (Wolf graft)
- Consists of the epidermis and full thickness of the dermis
- Harvested using an ordinary scalpel
- Needs excellent vascularity of the recipient wound for graft survival
- Used for small uncontaminated wounds produced after excision of skin lesions or after release of skin contractures (lower eyelids, fingers)


“Steps to explain types of skin grafts: Split-thickness vs full-thickness vs composite grafts: Q&A guide”
- The donor area needs primary suturing or split skin graft for healing and hence limits the size of the graft.
- Unlike split skin grafts, full-thickness grafts do not contract and retain its color and hence it is cosmetically superior.
Indications of skin graft
- Skin loss
- Post-traumatic (for example avulsion and degloving injury)
- Post-surgical (for example, excision of tumors, excision of burn wound)
- As a result of the pathological process. (example venous ulcer, diabetic ulcer)
- Mucosa loss
- After excision of lesions of the oral cavity, the tongue.
- For resurfacing reconstructed vagina in cases of vaginal agenesis.
Contraindications for skin graft
- Infection by beta-hemolytic Streptococcus, which produces fibrinolysis, which dissolves fibrin.
- Any nearby infected wound with copious discharge.
- Avascular wounds with exposed bare bone without periosteum, exposed tendon without paratenon and exposed cartilage without perichondrium.
Healing Of The Donor Area
The donor area of a split skin graft heals by epithelisation from the adnexal remnants of the dermis, pilosebaceous follicles, and/or sweat gland apparatus. Complete healing of the donor area occurs in 8–10 days.
The Process Of ‘Graft Take’
- The processes that result in reattachment and revascularization of the graft to the bed are collectively referred to as “take” of the graft.
- The graft initially adheres to its new bed by fibrin, and the revascularization, which starts in 48 hours and is completed in 4–5 days, is achieved by the outgrowth of capillary buds from the recipient area to unite with those on the deep surface of the graft. For the first 2 days after grafting, the skin graft derives its nutrition from the wound by the process of serum imbibition/ plasmatic circulation.
Ideal Requirements For Free Skin Graft
- Wound should be free from Infections like Streptococcus and Pseudomonas
- Vascular wounds, for example. wounds with healthy granulation
- The wound should be thoroughly debrided
- To achieve hemostasis before placing the graft
- To have close and immobile contact between the graft and the wound
- The recipient area should be immobilized with a POP slab
“Role of split-thickness grafts in covering large wounds: Questions answered”
Flaps
A flap is a block of tissue transferred from the donor to the recipient area with its integrated vascularity.
Common Indications Of The Flap Surgery
- To cover defects/wounds where a free skin graft cannot be used, for example. exposed bare bones, bare tendons, bare cartilage.
- Wounds with exposed joints expose major vessels and nerves.
- Implant exposure following orthopedic procedures.
- In wounds with soft tissue loss, future reconstructive surgery is contemplated.
- Defects that need better contour to improve cosmesis.
- Breast reconstruction following mastectomy.
Classification Of Flaps
- Broadly classified into pedicled flaps and free flaps
Pedicled Flaps: The pedicle or the base remains attached to the donor site during its transfer to the recipient area. Pedicled flaps may be of the following types.- Local flaps, for example, rotation, transposition, Limberg, and bilobed.
- Regional flap, for example, PMMC, DP for head and neck defects, and TRAM for breast reconstruction.
- Distant flaps, for example, the groin flap, and the subaxillary flap for hand defects.
Free Flaps: These are completely detached from the donor area before being transferred to the recipient area. The vascularity of the flap at the recipient site is immediately restored by anastomosing the vessels of the flap with the vessels at the recipient area using microvascular techniques.
- Based on the composition, the flaps may be classified as:
- Skin flap
- Fasciocutaneous flap
- Muscle flap
- Myocutaneous flap
- Adipofascial flap
- Osteocutaneous flap.
“How does full-thickness grafting improve aesthetic outcomes? FAQ explained”
Some Of The Commonly Performed Flaps
Forehead flap: Entire forehead skin can be raised based on an anterior branch of the superficial temporal artery. It bears an unsightly scar from the donor site. A median (Indian) forehead flap based on supratrochlear vessels is a very useful flap in reconstructing defects over the nose.
Deltopectoral flap (DP): It is supplied by the upper 4 perforating branches of the internal mammary artery, used to reconstruct the defects of the neck and lower face. After about 4 weeks, the flap is divided and the base is returned to the chest wall.
Pectoralis major myocutaneous (PMMC) flap: The pectoral branch of the thoracoacromial artery is the pedicle of the flap. It is the ideal pedicled flap for the reconstruction of head and neck defects following ablative surgeries for various head and neck cancers. Hence it is described as a workhorse among the flaps. Osteomyocutaneous PMMC flap including the 5th or 6th rib can be used for mandibular reconstruction.
Latissimus dorsi flap (LDF): As a myocutaneous flap, based on thoracodorsal vessels can be used for reconstruction of the lower half of the face, neck, breast, chest wall, axilla, and upper arm.

“Early warning signs of gaps in understanding skin graft types: Common questions”
Free (Microvascular) Flaps
Using an operating microscope and microvascular techniques, it is possible to do a free tissue transfer of tissues like skin, muscle, bone, intestine, omentum, etc. The procedure involves anastomosis of vessels of the flap to the vessels at the donor site, for example, Latissimus dorsi muscle myocutaneous flap, radial artery forearm flap, gracilis flap, free fibula flap, etc.
Electrical Burns
The most important factors taken into consideration while assessing the damage caused by the passage of electrical current through the body are—the nature of electric current and the resistance of body tissues through which the electric current is passing.
- When a portion of the body comes in contact with a live electric wire, the actual point where the electric current enters the body is known as the point of entry or is grounded as the point of exit. The most important factor which decides the severity of the injury is the “voltage” of the current.
- The resistance offered by the tissues to the flow of current leads to the conversion of electrical energy to thermal injury and hence tissue damage.

Electrical Burns: Types Of Injuries
True electrical injury: Damage is a result of heat generated due to the passage of current.
Flame burns: Due to an electrical flash or spark.
Arc burns: Localised injury due to intense heat at the termination of current flow. It occurs when it jumps the gap between the source and the conductor, for example, the flexor aspect of joints.
Electrical Burns Classification
1. Acute Injuries
Burn injuries due to electric current itself
“Asymptomatic vs symptomatic effects of ignoring grafting principles: Q&A”
- Low voltage injuries (Less than 1000 volts of current)
- Flash burns,
- Contact burn.
- High voltage injuries (More than 1000 volts of current)
- Flash,
- Arc or contact
- Punctate
- Extensive
- Extensive with vascular impairment of extremities.
- Compartment syndrome
- Dry gangrene
2. Other associated injuries
- Thermal burns due to ignited cloth
- Acute CNS problems
- Acute peripheral neuropathy
- Cardiac/respiratory arrest
- Injuries to other internal organs due to falls or electric current.
Delayed Injuries
- Delayed spinal cord injury
- Delayed peripheral neuropathy
- Optic nerve atrophy
- Cataract.
Chemical Burns
- Chemicals are a relatively uncommon cause of burns. The chemicals used in industry, science laboratories, and homes are the usual agents.
- The tissue damage in chemical burns is mainly due to the prolonged contact period and the effects of systemic absorption.
Classification Of Agents That Cause Injury
- Acids: Hydrochloric acid, sulphuric acid, nitric acid, hydrofluoric acid, phenol (carbolic acid), oxalic acid.
- Alkalis: Sodium hydroxide, potassium hydroxide, lithium, barium, ammonium hydroxide, and calcium hydroxide.
- Others: Inorganic substances: Phosphorus, wet cement lime, potassium permanganate, Organic substances: Kerosene, petrol, turpentine, naphthalene, etc.
“Can targeted interventions reduce risks of graft failure? FAQs provided”
Summary Of Management Of Electrical Injury
- Initial resuscitation as in thermal burns
- Low voltage injury
- Superficial—conservative
- Deep dermal—-tangential excision and split skin graft
- Contact burns—excision with SSG/flap
- High voltage injury
- Flash burns: Superficial—conservative
- Deep dermal: Tangential excision and split skin graft
- Arc or Contact burns: Vascular compromise— immediate
fasciotomy, amputation - Punctate wounds: Excision and grafting
- Extensive injury without vascular compromise: Wider excision with a split skin graft or flap cover
- The recipient area should be immobilized with a POP slab
Modes Of Action Of Chemicals On Tissues
- Acid causes coagulative necrosis of the skin due to rapid conversion of protein to coagulum salt of the acid.
- The coagulated eschar prevents these acids from penetrating deeply. Activity in the tissues continues for a long time.
- Alkalis are corrosive agents and produce extensive denaturation of tissue proteins. These produce more tissue destruction than acids.
First Aid
- Early irrigation of injured areas with large volumes of water or running water (with few exceptions) is the main focus in the first aid management of chemical injuries.
- Hydrotherapy mechanically cleans the area, reducing the concentration of chemicals and duration of contact. The earlier the hydrotherapy started, the more benefits were obtained.
- Since the absorption of phenol increases with dilution, surface phenol is removed by solvent polyethylene glycol before hydrotherapy is started.
Definitive Wound Closure
Achieved in a similar way as in any other thermal injury
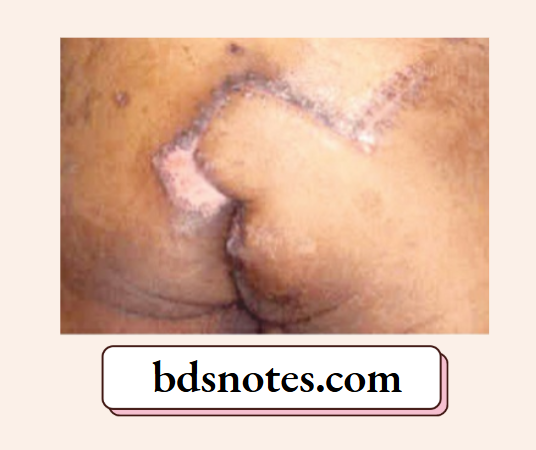
- Primary excision and split skin grafting, of all acid and alkali burns, if done within 10 days of the burns.
- Grafting of granulating wound, if the patient comes late, with a wound infection. This takes much longer (1½ months) compared to thermal burns (3 weeks).
“Differential applications of traditional vs modern grafting tools: Questions answered”
Ocular Injuries
Very common in acid and alkali burns. Severe blepharospasm and forceful rubbing increase the severity of the injury. Various sequences of events are:
- Sloughing of corneal epithelium
- Stromal edema
- Corneal ulceration
- Perforation
- Panophthalmitis
- If perforation does not occur, corneal opacity and heavy vascularization occur. Quick, thorough, and prolonged lavage of the cornea with water is the most important measure in first aid treatment. Systemic and topical steroids minimize inflammation and scarring of the cornea.
Leave a Reply