Management Of Osteomyelitis Of The Jaws
Write a short note on osteomyelitis.
Or
Write a short note on osteomyelitis of the jaw.
Answer. Osteomyelitis may be defined as an inflammatory condition of bone that begins as an infection of the medullary cavity and haversian system of the cortex and extends to involve the periosteum of the affected side.
Read And Learn More: Maxillofacial Fractures, Disorders, and Treatments
Osteomyelitis more frequently occurs in the mandible than in the maxilla.
Osteomyelitis Of The Jaws Management
“Emerging Treatments For Jaw Bone Infections”
Classification of Osteomyelitis
- Acute Osteomyelitis
- Acute suppurative osteomyelitis
- Acute subperiosteal osteomyelitis
- Acute periostitis.
- Chronic Osteomyelitis
- Nonspecific type:
- Chronic intramedullary osteomyelitis
- Chronic focal sclerosing osteomyelitis
- Chronic diffuse sclerosing osteomyelitis
- Chronic osteomyelitis with proliferative periostitis
- Chronic subperiosteal osteomyelitis
- Chronic periostitis.
- Specific type:
- Tuberculous osteomyelitis
- Syphilitic osteomyelitis
- Actinomycotic osteomyelitis.
- Nonspecific type:
- Radiationinduced osteomyelitis.
- Idiopathic osteomyelitis.
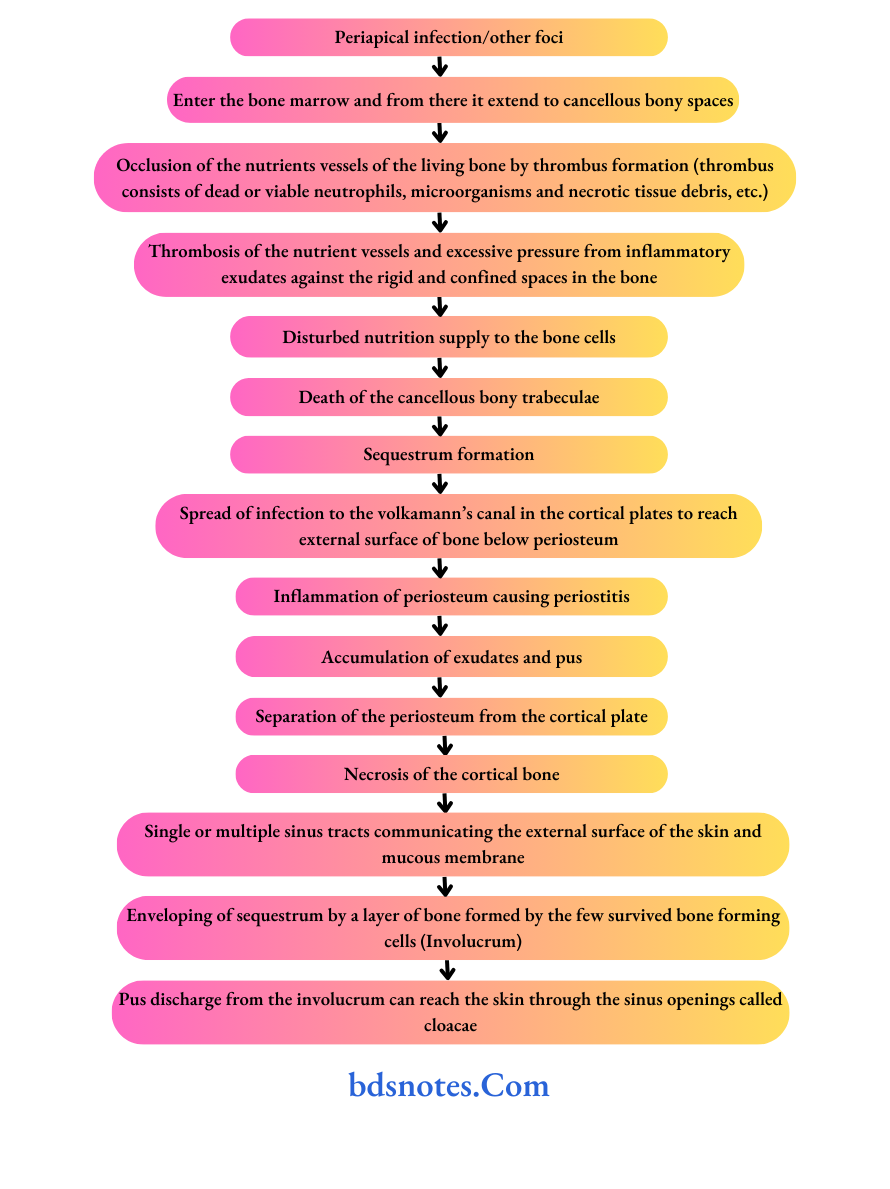
Osteomyelitis Pathogenesis
Osteomyelitis Clinical Features
- Pain and tenderness are minimal.
- Non-healing bony and overlying soft tissue wounds with indurations of soft tissues.
- Thickened or wooden character of bone.
- A history of chronic discharge in the oral cavity or on the face through the sinus is present.
- The pathological fracture may occur.
- Teeth in the area tend to become loose and sensitive to palpation and percussion.
- Lymphadenopathy is present.
Jaw Osteomyelitis Treatment
“Complications Of Untreated Jaw Osteomyelitis”
Osteomyelitis Treatment
“Acute Vs Chronic Osteomyelitis Of The Mandible”
Treatment of Acute Osteomyelitis
The treatment includes:
- Conservative treatment.
- Surgical treatment.
- The goal of management is
- Attenuate and eradicate proliferating pathology-
- cal organism.
- Promote healing.
- Re-establish vascular permeability.
- The goal of management is
Successful treatment based on
- Early diagnosis.
- Bacterial culture and sensitivity test.
- Adequate and prompt antibiotic therapy.
- Adequate pain control.
- Proper surgical intervention.
- Reconstruction (if indicated).
“Classification Of Jaw Osteomyelitis Types“
Chronic Osteomyelitis Of The Mandible
Conservative treatment
- Complete bed rest.
- Supportive therapy: It includes nutritional support in form of a high protein and high caloric diet and adequate multivitamins.
- Dehydration control: Hydration orally or through IV fluid.
- Blood transfusion: When RBC and Hb are low.
- Control of pain: Analgesic and sedation.
- Intravenous antimicrobial agents: Penicillin.

Surgical treatment
Surgical intervention is done under antibiotic cover, started at least 1 to 2 days before the procedure.
“Recovery After Jaw Osteomyelitis Surgery”
Incision And Drainage
- Done as soon as possible.
- It relieves pain and pressure caused by pus accumulation.
- Extraction of loose or offending teeth.
- Debridement: Followed by incision and drainage, thorough debridement of the affected area should be carried out.
- The area may be irrigated with hydrogen peroxide and saline thrice a day.
- Any foreign body, necrotic tissue, or small sequestrum should be removed.
- Drainage for the body and angle of the mandible area is established through an extraoral submandibular skin incision.
- Intraoral drainage can be established for the body of the mandible.
- Sequestrum formed should be removed, if it can be gently picked up (sequestrectomy).
Maxillary Osteomyelitis Treatment
Treatment of Chronic Osteomyelitis
Done by sequestrectomy and saucerization (removal of bony cavity).
“Role Of CT Scan In Jaw Bone Infection“
Surgical Management Of Jaw Osteomyelitis
Chronic Osteomyelitis Sequestrectomy
- Removal of sequestrum.
- It may be carried out under the proper cover of antibiotics.
- Small sequstrae are removed under local anesthesia.
- General anesthesia may be given for the removal of a larger sequestrum.
- Sequestra from the lower border of the mandible are best removed by extraoral approach using Risdon’s incision.
- From the ramus, it may be removed by retromandibular incision.
- From the condyle by preauricular incision.
- The coronoid process is best approached by an oral incision given along the anterior border of the ramus of the mandible.
- After removal of the sequestrum, the residual granulation tissue is curetted till white shining bone appears.
- Bleeding is controlled by a pressure pack.
- When complete infection has been eradicated, the wound can be closed by primary closure.
- When the elimination of the infection is doubtful, a glove drain or a rubber drain is kept in place and is changed every 24 hours till no discharge from the bone, is seen.
“Pain Management For Jaw Osteomyelitis”
Antibiotics For Jaw Osteomyelitis
Chronic Osteomyelitis Saucerization
- Removal of bony cavity.
- It consists of elimination for bony cavity in the jaw bone to avoid collection of blood and formation of large hematoma which is liable to get infected.
- It is a simple procedure for eliminating the dead space inbone.
- Saucerization is carried out by existing the wall of the bony cavity by means of Rongeur bone-cuttng forceps or burs.
- The bone is smoothed by a file.
- The wound can be partially or completely closed depending on the amount of suppuration.
Leave a Reply