A Comprehensive Overview of Radicular (Periapical) Cyst
Question. Classify cysts of the oral region. Discuss the radicular cyst in detail.
Or
Write a note on the radicular cyst.
Or
Write a short note on the radicular cyst.
Or
Classify odontogenic cyst. Describe the pathogenesis, clinical, radiological, and histopathological features of radicular cyst.
Answer.
Radicular Cyst
- It is also called an apical periodontal cyst or periapical cyst, or dental root end cyst.
- It is an inflammatory odontogenic epithelial cyst.
- It is a common sequela in progressive changes associated with bacterial invasion and death of the dental pulp.
- It most commonly occurs at the apices of the teeth.
“Understanding the role of radicular cysts in dental pathology: Q&A explained”
Pathogenesis Of Radicular Cyst
Radicular cyst develops due to the proliferation and subsequent cystic degeneration of the “epithelial cell rests of Malassez”, in the periapical region of a nonvital tooth.
The process of development of this cyst occurs in various stages:
- Phase of initiation
- Phase of proliferation
- Phase of mystification
- Phase of enlargement
“Importance of studying radicular cysts for better diagnostic outcomes: Questions explained”
- Phase of initiation: During this phase, the bacterial infection of the dental pulp or direct inflammatory effect of necrotic pulpal tissue, in a nonvital tooth, causes stimulation of the “cell rest of Malassez,” which are present within the bone near the root apex of teeth.
- The phase of proliferation: The stimulation to the Malassez rests of Malassez leads to excessive proliferation of these cells, which leads to the formation of a large mass or island of immature proliferating epithelial cells at the periapical region of the affected tooth.
- Phase of certification: Once a large bulk of the cell rest of Malassez is produced, its peripheral cells get adequate nutritional supply but its centrally located cells are often deprived of proper nutritional supply. As a result, the central group of cells undergoes ischemic liquefactive necrosis while the peripheral group of cells survives. This eventually gives rise to the formation of a cavity that contains a hollow space or lumen inside the mass of the proliferating cell rest of Malassez and a peripheral lining of epithelial cells around it.
- Phase of enlargement: Once a small cyst is formed, it enlarges gradually by the following mechanisms:
- Higher osmotic tension of the cystic fluid causes a progressive increase in the amount of fluid inside its lumen and this causes increased internal hydrostatic tension within the cyst. The process results in cyst expansion due to resorption of the surrounding bone.
- The epithelial cells of the cystic lining release some bone resorbing factors like prostaglandins and collagenase, etc. which destroy the bone and facilitate expansion of the cyst.
“Common challenges in diagnosing radicular cysts effectively: FAQs provided”
Clinical Features
- It most commonly occurs on 3rd, 4th, and 5th decades of life.
- It is more common among the males.
- Maxillary anteriors are most commonly affcted.
- Majority of cases are asymptomatic.
- It is associated with the nonvital tooth.
- Small cystic lesions are asymptomatic.
- Large lesions often produce a slow enlarging bony hard swelling of the jaw with expansion of cortical plates.
- Severe bone destruction produces “springiness” of jaw bone.
- If the cyst is secondarily infected it leads to the formation of the abscess, which is called “cyst abscess”.
“Steps to explain the formation of radicular cysts: Inflammation vs necrosis: Q&A guide”
Histological Features
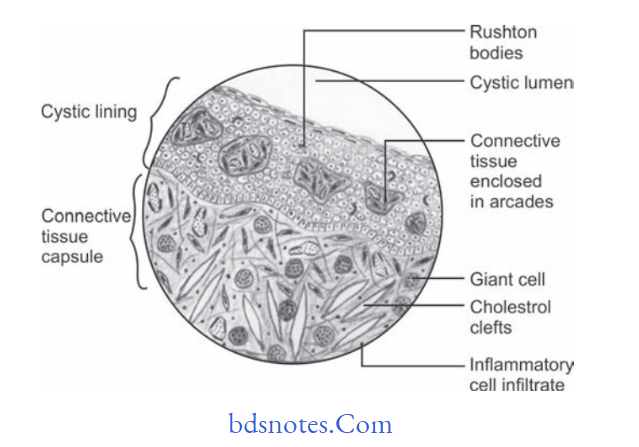
“Role of periapical infection in radicular cyst development: Questions answered”
- Radicular cyst is lined by the stratifid squamous epithelium.
- It is lined by pseudostratifid, columnar or respiratory
type Of Epithelium. - Hyaline bodies or Rushton bodies often found in the great numbers in the epithelium of apical periodontal cyst.
- Collagenous connective tissue makes the wall of radicular cyst.
- Abundant firoblast can be identifid within the cystic wall.
- Cystic wall presents inflmmatory infitrate which contains lymphocytes, plasma cells.
- Other histological fidings within the cyst wall are erythrocytes, area of hemorrhage, occasional spicules of dystrophic bone, multinucleated giant cells and cholesterol crystals.
“Early warning signs of issues addressed by understanding radicular cyst pathogenesis: Common questions”
Radiological Features
It is round or oval radiolucency of variable size which is generally well delineated and is most likely with marked radiopaque rim.
Treatment
Root canal treatment
Extraction of involved tooth
Enucleation or marsupialization of large lesion is done.
Leave a Reply