Type IV Hypersensitivity
Define and classify hypersensitivity reactions. Discuss Type 4 (delayed hypersensitivity) in brief.
Or
Write a short note on type 4 hypersensitivity reaction.
Or
Write a brief on the delayed type of hypersensitivity.
Or
Write a note on the delayed type of hypersensitivity.
Answer:
Hypersensitivity is defined as a state of exaggerated immune response to an antigen.
Classification By Coomb and Gel (1963)
- Immediate Type
- Type 1: Anaphylactic, atopic reaction
- Type 2: Cytotoxic reaction
- Type 3: Immune complex reaction.
- Delayed Type
- Type 4: Cell-mediated reaction
- Later on, Type 5 hypersensitivity reaction was also described, i.e. stimulatory type.
Type IV hypersensitivity examples
Type 4 (Delayed Hypersensitivity)
Type 4 hypersensitivity reaction is also known as delayed hypersensitivity or T cell-mediated reaction.
- The reaction is mediated by sensitized T-lymphocytes which, on contact with a specific antigen, release lymphokines that cause biological effects on macrophages, leucocytes, and tissue cells.
- Type 4 or delayed type of hypersensitivity occurs within 48-72 hours of antigen challenge. As it is not antibody-mediated, it cannot be passively transferred by serum but can be transferred by lymphocytes or the transfer factor.
Type 4 hypersensitivity Pathogenesis
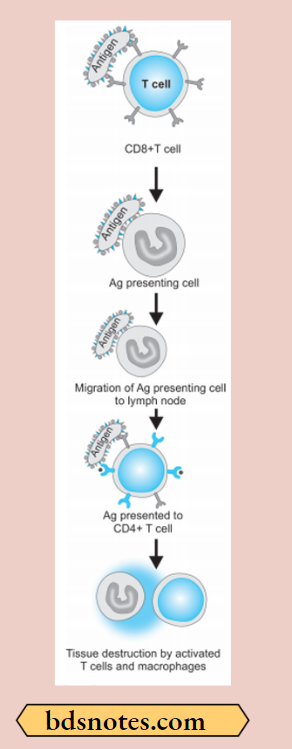
Type 4 reaction involves the role of mast cells and basophils, macrophages, and CD8+ T cells. Briefly, the mechanism of the type 4 reaction is as under:
- The antigen is recognized by CD8+ T cells (cytotoxic T cells) and is processed by antigen-presenting cells.
- Antigen-presenting cells migrate to lymph nodes where antigen is presented to helper T cells (CD4+ T cells).
- Helper T cells release cytokines that stimulate T cell proliferation and activate macrophages.
- ActivatedTcellsandmacrophagesreleaseproinflmmatory mediators and cause cell destruction.
Types of Delayed Hypersensitivity
Two types of delayed hypersensitivity reactions are well recognized, the tuberculin (infection) type and the contact dermatitis type.
Tuberculin (Infection) Type
- When a small dose of tuberculin is injected intradermally in an individual sensitized to tuberculoprotein by prior infection or immunization, an erythema and swelling (induration) occur at the site of injection within 48-72 hours.
- The injection site is infiltrated by a large number of lymphocytes and about 10-12% macrophages.
- In unsensitised individuals, the tuberculin injection provokes no response.
- Purified protein derivative (PPD) which is the active material of tubercle bacilli, is used in tuberculin tests.
- The tuberculin test is a useful indicator for delayed hypersensitivity to the bacillus.
- Cell-mediated hypersensitivity reaction develops in many infections with bacteria (M. tuberculosis, M. leprae), fungi, and parasites.
- It occurs when the infection is subacute or chronic and the pathogen is intracellular.
- Various skin tests are performed to detect delayed types of hypersensitivity.
- A positive skin test does not indicate a present infection but implies the person has been infected or immunized by microorganisms in the past. Some of these skin tests include:
- Lepromin test: It is positive in tuberculoid leprosy but negative in the lepromatous type of leprosy.
- Frei test: This test is positive in lymphogranuloma venereum (LGV).
- Histoplasmin test: It is positive in histoplasmosis.
Delayed-type hypersensitivity mechanism
Contact Dermatitis Type
- Delayed hypersensitivity may sometimes develop as a result of skin contact with a range of sensitizing materials metals such as nickel and chromium, drugs such as penicillin or other antibiotics in ointments, simple chemicals like hair dyes, picryl chloride, dinitrochlorobenzene, cosmetics, and soaps.
- These substances can act as haptens.
- After absorption through the skin, these molecules combine with skin protein to become antigenic.
- Cell-mediated immunity is induced in the skin.
- As most of the antigens involved are fat soluble, their likely portal of entry is along the sebaceous glands.
- Sensitization is particularly liable to occur when the chemical is applied in an oily base (ointment or cream) on an inflamed area of the skin.
- The Langerhans cells of the skin carry these antigens to regional lymph nodes where T-lymphocytes are sensitized.
- On subsequent exposure to the offending agent, sensitized lymphocytes release lymphokines which cause superficial inflammation of the skin characterized by redness, induration, and vesiculation within 24-48 hours.
- The dermis is infiltrated predominantly by lymphocytes and a few macrophages.
Morphology of Classic Delayed Hypersensitivity
- There is an accumulation of mononuclear cells around small veins and venules producing perivascular cuffing.
- Presence of increased microvascular permeability
- Escape of plasma proteins leading to dermal edema or deposition of fibrin in the interstitium (induration)
- Fully developed lesions show endothelial hypertrophy and hyperplasia.
- There are persistent/non-degradable antigens that induce perivascular lymphocytic infiltrate replaced by macrophages in 2 to 3 weeks. Macrophages are converted into epithelioid cells, which aggregate to form granulomas.
Leave a Reply