Type II Hypersensitivity
Write a brief note on Type 2 hypersensitivity reaction.
Answer:
Type 2 hypersensitivity reaction is also known as antibody-mediated reaction or cytotoxic reaction.
It is defined as a reaction by humoral antibodies that attack cell surface antigens on the specific cells and tissues and cause lysis of target cells. Type 2 reaction too appears generally within 15-30 minutes after exposure to an antigen, but in myasthenia gravis and thyroiditis, it may appear after a long duration.
Type 2 hypersensitivity Pathogenesis
Type 2 reactions are mediated by the complement system, tissue macrophages, platelets, natural killer cells, neutrophils, and eosinophils, while the main antibodies are IgG and IgM class.
Type 2 hypersensitivity is tissue-specific, and the reaction occurs after antibodies bind to tissue-specific antigens, most often on blood cells.
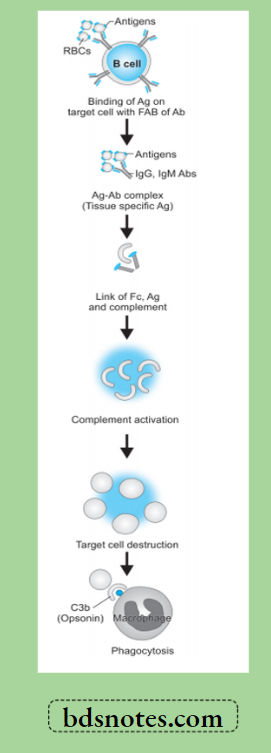
The mechanism involved is as under:
- The antigen on the surface of the target cell (foreign cell) attacks and binds the Fab portion of the antibody (IgG or IgM) forming the antigen-antibody complex.
- The unattached Fc fragment of antibodies (IgG or IgM) forms a link between the antigen and complement.
- The antigen-antibody binding with forming link causes activation of the classical pathway of serum complement which generates activated complement component, C3b by splitting C4 and C2 by C1.
- Activated C3b bound to the target cell acts as an opsonin and attacks phagocyte at the site of cell injury and initiates phagocytosis.
- Antigen—antibody complex also activates the complement system and exposes membrane attack complex (MAC i.e. C5b—C9) that attacks and destroys the target cell.
Type II Hypersensitivity
Examples of Type 2 Hypersensitivity Reaction
Examples of type 2 reactions are mainly on blood cells and some other body cells and tissues.
1. Cytotoxic Antibodies to Blood Cells
These are more common. Some examples are as under:
- Autoimmune hemolytic anemia in which the red cell injury is brought about by
autoantibodies reacting with antigens present on the red cell membrane. The antiglobulin test (direct Coombs test) is employed to detect the antibody on the red cell surface. - Transfusion reactions due to incompatible or mismatched blood transfusion.
- Hemolytic disease of the newborn i.e. erythroblastosis fetalis in which the fetal red cells are destroyed by maternal isoantibodies crossing the placenta.
- Immune thrombocytopenic purpura is the immunologic destruction of platelets by autoantibodies reacting with the surface components of normal platelets.
Epinephrine in anaphylaxi
2. Cytotoxic Antibodies to Tissue Components
Cellular injury may be brought about by autoantibodies reacting with some components of tissue cells in certain diseases.
- In Graves’ disease (primary hyperthyroidism), thyroid autoantibody is formed which reacts with the TSH receptor to cause hyperfunction and proliferation.
- In myasthenia gravis, antibody to acetylcholine receptors of skeletal muscle is formed which blocks the neuromuscular transmission at the motor end plate, resulting in muscle weakness.
- In male sterility, the anti-sperm antibody is formed which reacts with spermatozoa and causes impaired motility as well as cellular injury.
- In type 1 diabetes mellitus, islet cell autoantibodies are formed which react against islet cell tissue.
Leave a Reply