Osteomyelitis
Discuss in briefly osteomyelitis.
Or
Discuss etiopathogenesis and morphological changes in pyogenic osteomyelitis.
Answer:
Osteomyelitis is defined as an inflammation of the soft tissue components of the bone which includes bone marrow, haversian canals, and periosteum with secondary changes in the mineralized components of the bone.
Osteomyelitis Etiopathogenesis
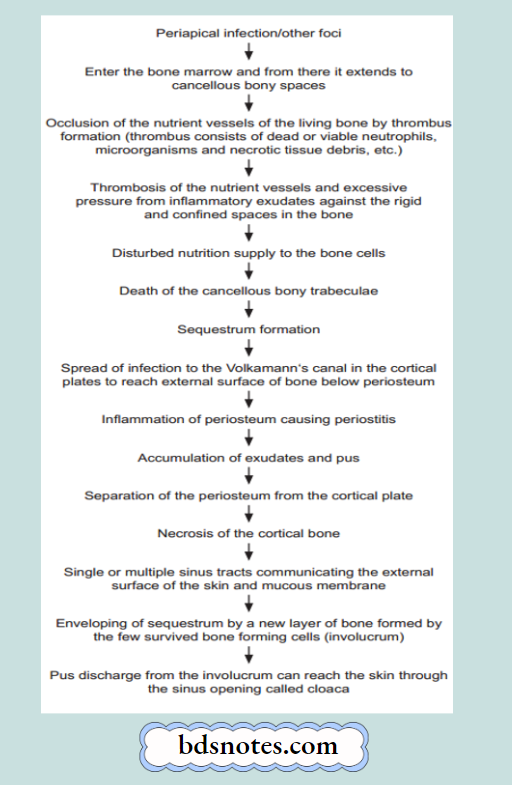
Morphological Changes in Pyogenic Osteomyelitis
- The morphologic changes in osteomyelitis depend on the stage (acute, subacute, or chronic) and the location of the infection.
- Infection begins at the metaphyseal end of the marrow cavity which is occupied by pus.
- Tension in the marrow cavity is increased because of the presence of pus and leads to the spread of infection along the marrow cavity, into the endosteum, and the Haversian and Volkmann’s canal, causing periosteitis.
Osteomyelitis
- The infection may reach the subperiosteal space forming subperiosteal abscesses. It may penetrate through the cortex forming draining skin sinus tracts.
- A combination of suppuration and impaired blood supply to the cortical bone leads to erosion, thinning, and infarction necrosis of the cortex called a sequestrum.
- Along with time, there is the formation of new bone beneath the periosteum present over the infected bone. This forms an encasing sheath around the necrosed bone and is known as an involucrum. The involucrum has an irregular surface and has perforations through which discharging sinus tracts pass.
- Long-continued neo-osteogenesis gives rise to a dense sclerotic pattern of osteomyelitis called chronic sclerosing nonsuppurative osteomyelitis of Garré.
- Occasionally, acute osteomyelitis may be confined to a localized area and walled off by fibrous tissue and granulation tissue. This is termed Brodie’s abscess.
- In vertebral pyogenic osteomyelitis, the infection begins from the disc (discitis) and spreads to involve the vertebral bodies.
Leave a Reply