Osteomyelitis
Question 1. Define and classify osteomyelitis. Describe in detail chronic osteomyelitis.
Or
Write short note on chronic osteomyelitis.
Answer.
Chronic Osteomyelitis
Chronic osteomyelitis is the persistent abscess of the bone characterized by a complex inflammatory process, including necrosis of mineralized and marrow tissues, suppuration, resorption, sclerosis, and hyperplasia.
Osteomyelitis is defined as an inflammatory condition of bone that begins as an infection of the medullary cavity and haversian systems of the cortex and extends to involve the periosteum of the affected area.
osteomyelitis
“Role of Staphylococcus aureus in osteomyelitis”
Classification of Osteomyelitis
- Acute osteomyelitis
- Acute suppurative osteomyelitis
- Acute subperiosteal osteomyelitis
- Acute periostitis
- Chronic osteomyelitis
- Non-Specific Type
- Chronic intramedullary osteomyelitis
- Chronic focal sclerosing osteomyelitis
- Chronic diffuse sclerosing osteomyelitis
- Chronic osteomyelitis with proliferative periostitis
- Chronic subperiosteal osteomyelitis
- Chronic periostitis
- Specific type
- Tuberculous osteomyelitis
- Syphilitic osteomyelitis
- Actinomycotic osteomyelitis
- Non-Specific Type
- Radiation-induced osteomyelitis
- Idiopathic osteomyelitis
“Symptoms of osteomyelitis in adults”
Pathogenesis
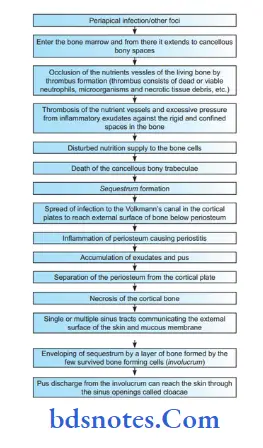
“Pain and swelling in osteomyelitis explained”
Clinical Features
- The molar area of the mandible is more frequently affected.
- Pain is usually mild and insidious and is not related to the real severity of the disease.
- Jaw swelling is a common feature, but mobility of teeth and sinus tract formation are rare.
- Anesthesia and paresthesia of the lip are uncommon.
- Regional lymphadenopathy is common.
- There is a thickened, woodened feeling of bone and a slow increase in jaw size.
“Pathophysiology of osteomyelitis explained”
Histopathology
- Chronic inflammatory reaction of bone with accumulation of exudate and pus within medullary spaces.
- Lymphocytes, macrophages, and plasma cells predominate among the inflammatory cells.
- Osteoblastic and osteoclastic cavity occurs partially with formation of irregular bony trabeculae having reversal lines.
- Sequestrum may develop in later stages of the disease.
Colonies of bacteria are also seen within the inflamed tissue.
chronic osteomyelitis
“Role of imaging in osteomyelitis diagnosis”
Question 2. Describe briefly the etiology of pulpitis.
Answer. The following is the etiology of pulpitis
- Dental caries that extend beyond the dentinal barrier and reach pulp lead to pulpitis.
- During cavity preparation, if pulp exposure occurs, this will lead to pulpitis.
- When a blow to the tooth occurs, it leads to damage to the pulp.
- If cavity preparation is done without using the water spray this lead to the excessive heat production to tooth which lead to pulpitis.
- Chemical irritation to pulp
- Cracked tooth syndrome
- If metallic restoration is given in the tooth without providing proper thermal insulation, this will lead to pulpitis.
Leave a Reply