Mechanism of Invasion and Metastasis Notes
“What is the mechanism of invasion and metastasis in cancer?”
Neoplasia is defined as a mass of tissue formed as a result of the abnormal, excessive, uncoordinated, autonomous, purposeless proliferation of cells even after cessation of stimulus for growth which caused it.
Enumeration of Pathways of Metastasis
The following are the pathways of metastasis:
- Lymphatic spread.
- Hematogenous spread.
- Other routes:
- Transcelomic route
- Spread through epithelial-lined surfaces
- Spread via CSF
- Implantation.
“Understanding the role of invasion and metastasis in cancer progression”
“Importance of studying invasion and metastasis for better cancer outcomes”
Mechanism of Invasion and Metastasis
The following steps are involved at the molecular level which explains the mechanism of invasion and metastasis:
1. Aggressive clonal proliferation and angiogenesis: The first step in the spread of cancer cells is the origin of rapidly proliferating clones of cancer cells.
This is explained on the basis of tumor heterogeneity, i.e. in the population of monoclonal tumor cells, a subpopulation or clone of tumor cells has the right biologic characteristics to complete the steps involved in the development of metastasis.
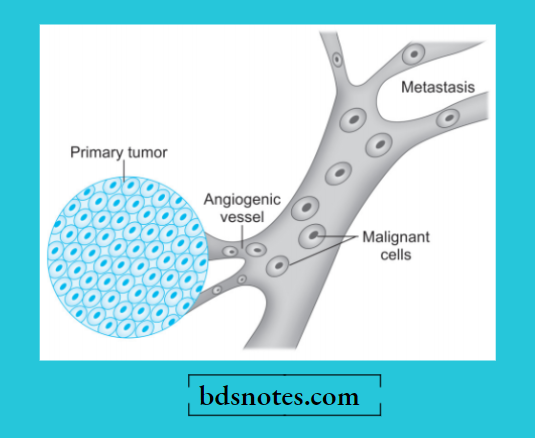
Tumor angiogenesis plays a very important role in metastasis as the new vessels formed are part of growing tumors and are more vulnerable to invasion as these originating vessels are directly in contact with cancer cells.
“Common challenges in understanding invasion and metastasis mechanisms”
2. Tumor cell loosening: Normal cells remain attached to each other due to the presence of cell adhesion molecules, i.e. E (epithelial), and cadherin. In epithelial cancers, there is either loss or inactivation of E-cadherin and also other cell adhesion
molecules of the immunoglobulin superfamily, all of which lead to the loosening of cancer cells.
3. Tumor cell-ECM interaction: Loosened tumor cells are now attached to extracellular matrix proteins, i.e. laminin and fibronectin. This attachment gets facilitated because of the pro- fondness of receptors on the cancer cells for both these proteins. There is also a loss of integrins, the transmembrane receptors, further favoring invasion.
4. Degradation of ECM: Tumor cells overexpress proteases and matrix-degrading enzymes, metalloproteinases, i.e. collagenases and gelatinase, while the inhibitors of metalloproteinases are decreased.
Another protease, cathepsin D, is also increased in certain cancers. These enzymes cause the dissolution of the extracellular matrix. Firstly basement membrane of the tumor itself, then they make way for tumor cells through the interstitial matrix and finally dissolve the basement membrane of the vessel wall.
“Steps to explain the mechanisms of cancer cell invasion”
5. Entry of tumor cells into capillary lumen: Tumor cells after degrading the basement membrane are ready to migrate into the lumen of capillaries or venules for which the following mechanisms play a role:
- The autocrine motility factor is a cytokine derived from tumor cells and stimulates receptor-mediated motility of tumor cells.
- Cleavage products of matrix components that are formed following the degradation of extracellular matrix have properties of tumor cell chemotaxis, growth promotion, and angiogenesis in cancer. After the malignant cells have migrated through the breached basement membrane, these cells enter the lumen of lymphatic and capillary channels.
6. Thrombus formation: Tumor cells protruding in the lumen of the capillary get covered with constituents of the collating blood and form the thrombus. Thrombus provides nourishment to the tumor cells and also protects them from the immune attack by the circulating host cells.
In fact, normally a large number of tumor cells are released into circulation but they are attacked by the host immune cells. Actually, a very small proportion of malignant cells in the bloodstream survive to develop into metastasis.
“Role of epithelial-to-mesenchymal transition (EMT) in tumor invasion”
7. Extravasation of tumor cells: Tumor cells in the circulation may mechanically block the vascular channels and attach vascular endothelium. In this way, the sequence similar to local invasion is repeated and the basement membrane gets exposed.
8. Survival and growth of metastatic deposit: Extravasated malignant cells on lodgement in the risk environment grow further under the influence of growth factors produced by host tissues, tumor cells, and cleavage products of matrix components. These growth factors in particular include:
PDGF, FGF, TGF-β, and VEGF. The metastatic deposits grow further if the host’s immune defense mechanism fails to eliminate them. Metastatic deposits may further metastasize to the same organ or to another site by forming emboli.
“Early warning signs of untreated invasive cancer behaviors”
Summary of Invasion and Metastasis
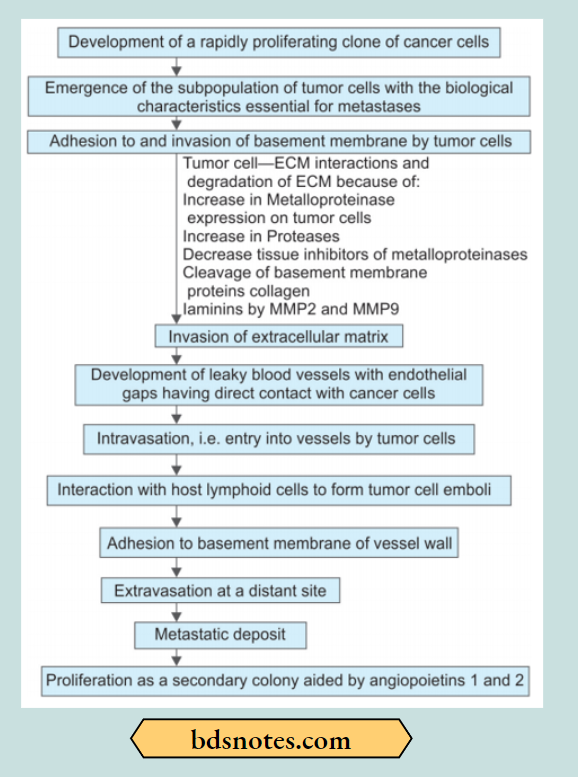
“Asymptomatic vs symptomatic stages of cancer invasion progression”
Leave a Reply