Extraoral Anchorage Advantages
- Anchorage established from an extraoral anchorage source is much greater than an introral anchorage source since extraoral anchorage units are more stable.
- There is a lower risk of anchor loss.
Anchorage is a key concept in orthodontics, referring to the resistance against unwanted tooth movement during treatment. Understanding how to define and classify anchorage is crucial for orthodontists to achieve the desired outcomes for their patients. This guide will break down the various aspects of anchorage, including its importance, classifications, techniques, and the latest advancements in the field.
“Understanding the role of anchorage in orthodontic treatment”
Orthodontics Key Significance
- Anchorage is the resistance against tooth movement during orthodontic treatment.
- It can be classified based on how force is applied, the jaws involved, and the site of anchorage.
- Techniques for anchorage include intraoral and extraoral methods, as well as absolute anchorage using implants.
- Effective anchorage management is vital to prevent unwanted tooth movement and ensure successful treatment outcomes.
- Recent technological advancements are improving anchorage control, making treatments more efficient.
“Importance of studying anchorage for better orthodontic outcomes”
Understanding Anchorage In Orthodontics

“Common challenges in defining and classifying anchorage effectively”
Definition Of Anchorage
So, what exactly is anchorage in orthodontics? Well, it’s basically about keeping certain teeth from moving when you’re trying to move others. Think of it as the anchor that prevents unwanted movement. It’s the resistance to displacement offered by teeth, bone, or even extraoral appliances when we apply force to shift other teeth. Without good anchorage, you might end up moving the wrong teeth, or moving teeth in the wrong direction. It’s a pretty big deal.
Importance of Anchorage In Treatment
Why is anchorage so important? Imagine trying to pull a wagon without anything to brace yourself against – you’d just slide backward! It’s the same with teeth. If you don’t have adequate orthodontic anchorage, you risk losing the position of your anchor teeth, which can mess up the whole treatment plan.
“Steps to explain the definition of anchorage in orthodontics”
Here’s why it matters:
- Predictable tooth movement: Anchorage helps ensure that the teeth you want to move are the ones that actually move.
- Efficient treatment: By preventing unwanted movement, anchorage can shorten the overall treatment time.
- Improved outcomes: Proper anchorage leads to better alignment, bite correction, and overall aesthetics.
Anchorage is not just a technical detail; it’s a cornerstone of successful orthodontic treatment. Careful planning and execution of anchorage strategies are essential for achieving the desired results and avoiding complications.
Factors Influencing Anchorage
Okay, so what affects how much anchorage you have? Several things come into play. Tooth size and root surface area are big factors – bigger teeth with longer roots generally provide better anchorage. Bone density around the teeth also matters; denser bone offers more resistance. The number of teeth used for anchorage is important too; using more teeth spreads the force and reduces the risk of individual tooth movement. Even things like the patient’s bite and muscle strength can have an impact. It’s a complex puzzle, and orthodontists need to consider all these factors when planning treatment.
Here’s a quick rundown:
“Role of anchorage in controlling tooth movement during treatment”
- Tooth size and root morphology
- Bone density
- Number of anchorage teeth
- Magnitude and direction of force
- Occlusal forces
Classifications Of Anchorage
Anchorage isn’t just a single concept; it’s a multifaceted aspect of orthodontic treatment. To better understand and manage it, we break it down into different categories. These classifications help orthodontists plan treatments more effectively and predict potential challenges.
Based on Force Application
This classification looks at how the force is being applied and how the teeth are responding. It’s all about understanding the mechanics at play.
- Simple Anchorage: This relies on the resistance of one or more teeth to move another tooth. Think of it as a straightforward tug-of-war.
- Stationary Anchorage: Here, the goal is to keep the anchorage unit absolutely still while moving other teeth. This often requires more robust anchorage methods.
- Reciprocal Anchorage: This involves moving two sets of teeth towards each other, using each set as anchorage for the other. It’s a balanced approach where both sides contribute.
Based on Jaws Involved
This classification considers whether the anchorage is within a single jaw or involves both jaws. It’s a simple but important distinction.
- Intramaxillary Anchorage: The anchorage and the tooth movement both occur within the same jaw (either the upper or lower).
- Intermaxillary Anchorage: This uses teeth in one jaw to provide anchorage for tooth movement in the opposite jaw. Elastics connecting the upper and lower arches are a common example.
Based on Site of Anchorage
This classification focuses on where the anchorage is derived from – what structures are providing the resistance?
- Intraoral Anchorage: This uses structures within the mouth, such as teeth, alveolar bone, or even the palate, to provide anchorage. It’s the most common type.
- Extraoral Anchorage: This utilizes structures outside the mouth, like the skull or neck, to provide anchorage. Headgear is a classic example of extraoral anchorage. These are less common now but can be useful in certain situations.
- Skeletal Anchorage: This involves using temporary anchorage devices (TADs), like mini-screws or mini-plates, that are anchored directly into the bone. These provide absolute anchorage methods and are becoming increasingly popular.
Understanding these classifications is key to successful orthodontic treatment. By carefully considering the type of anchorage being used, orthodontists can minimize unwanted tooth movement and achieve predictable results.
Types Of Anchorage Techniques
“Early warning signs of untreated issues related to anchorage”

“Asymptomatic vs symptomatic effects of improper anchorage definition”
Orthodontic treatment relies heavily on anchorage to achieve predictable tooth movement. Different techniques have evolved over time, each with its own set of advantages and disadvantages. The selection of an appropriate anchorage technique is crucial for successful treatment outcomes. Let’s explore the common types.
Intraoral Anchorage Techniques
Intraoral anchorage uses teeth and/or the alveolar bone within the patient’s mouth as the source of resistance. This is probably the most common type of anchorage we see.
- Simple Anchorage: This involves using a single tooth or a small group of teeth to resist movement. It’s often used for minor tooth corrections.
- Compound Anchorage: Here, a larger group of teeth is used to provide greater resistance. Think of it as teaming up to hold the line.
- Reciprocal Anchorage: This is when two teeth or groups of teeth are used to move each other. It’s like a tug-of-war where both sides are equally strong. For example, arch expansion using a midline screw.
Intraoral anchorage is convenient because it doesn’t require any extraoral appliances. However, it can be challenging to maintain, especially when significant tooth movement is required.
Extraoral Anchorage Techniques
Extraoral anchorage utilizes structures outside the mouth, such as the head or neck, to provide resistance. Headgear is a classic example of this. It’s not as common these days, but it still has its place.
- Headgear: This appliance applies force to the teeth and jaws from outside the mouth, typically using a strap around the head or neck. It’s often used to correct severe overbites or underbites.
- Cervical Anchorage: This type uses a neck strap to provide a pulling force, often used to restrain forward movement of the upper jaw.
- Occipital Anchorage: This involves using a head cap that rests on the back of the head to provide anchorage. It’s generally used for more significant corrections.
Absolute Anchorage Methods
Absolute anchorage aims to eliminate any unwanted tooth movement during orthodontic treatment. This is where things get interesting with modern technology. The most common method involves the use of temporary anchorage devices (TADs).
- TADs (Temporary Anchorage Devices): These are small screws or mini-implants that are surgically placed into the bone to provide a stable point of anchorage. They offer predictable and reliable resistance, allowing for more complex tooth movements. They are strategically placed in the jawbone to provide stable anchorage for tooth movement, enhancing the effectiveness of orthodontic procedures.
- Dental Implants: In some cases, dental implants can be used as a source of absolute anchorage. This is typically done in adults who are missing teeth and require significant tooth movement.
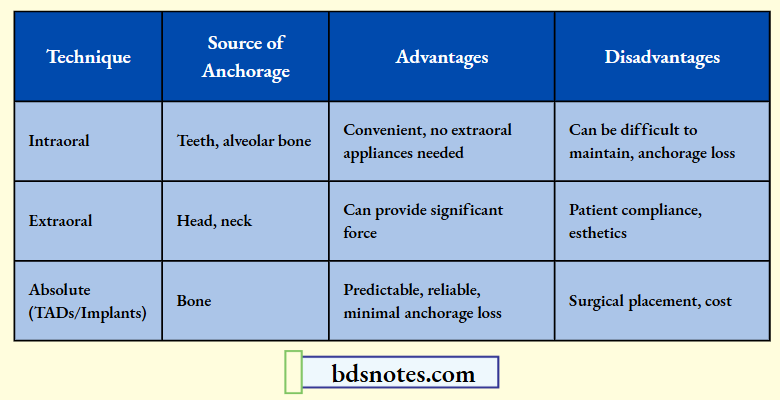
Here’s a quick comparison of the different anchorage techniques:
“Steps to educate patients about anchorage and its importance”
“Role of counseling in clarifying anchorage goals for patients”
Anchorage Planning And Management
Assessing Anchorage Requirements
Okay, so before you even think about moving teeth, you gotta figure out how much anchorage you’re gonna need. It’s like planning a road trip – you need to know how far you’re going before you pack the car. This means looking at a few things:
- How many teeth are we moving, and how far?
- Which teeth are easier to move than others?
- What’s the patient’s bite like to begin with?
Basically, we’re trying to predict how much resistance we’ll need to keep some teeth still while we move others. If you’re only making small adjustments, you might not need much. But if you’re doing some serious shifting, you’ll need a solid plan.
Strategies to Prevent Anchorage Loss
Anchorage loss is a pain. It’s when the teeth you’re trying to keep still start moving too. It’s like trying to push a car forward, but the parking brake isn’t fully on – frustrating! Here are some ways to avoid it:
- Use more teeth for anchorage. The more, the merrier!
- Consider using implants or temporary anchorage devices (TADs) for extra support.
- Make sure your mechanics are spot-on. Bad forces can lead to unwanted movement.
Think of it like this: you’re building a fence. You need strong posts to keep the fence stable. Anchorage is like those posts – the stronger they are, the better the fence (or your treatment) will hold up.
Reinforcement Techniques for Anchorage
Sometimes, you need to bring in the big guns. Reinforcing anchorage is like adding extra support beams to a house – it makes everything stronger. Here are a few techniques:
- Lingual Arches: These connect teeth on the inside of the mouth for added stability.
- Nance Appliance: This uses an acrylic button on the roof of the mouth to help hold molars in place.
- Transpalatal Arch (TPA): Similar to a lingual arch, but it connects molars across the palate.
These methods help distribute the forces and prevent individual teeth from bearing the brunt of the movement. It’s all about teamwork!
Recent Advances In Anchorage Control
Innovations in Anchorage Devices
Things are changing fast in orthodontics, especially when it comes to anchorage. We’re not just relying on headgear anymore! The development of temporary anchorage devices (TADs) has really revolutionized how we control tooth movement. These mini-implants or mini-screws provide a stable point to pull from, without depending on other teeth. It’s pretty cool.
- Improved TAD designs are making them easier to place and more comfortable for patients.
- Bioactive coatings on TADs are being explored to improve osseointegration.
- Smaller diameter TADs are becoming available, allowing for placement in more locations.
Impact of Technology on Anchorage
Technology is making a big difference. Digital planning software lets orthodontists predict tooth movement with greater accuracy. This means we can plan anchorage strategies better than ever before. 3D printing is also playing a role, allowing for custom-made anchorage appliances that fit perfectly and deliver forces exactly where they’re needed.
Using digital models and CBCT scans, orthodontists can now simulate treatment outcomes and adjust anchorage plans before even starting treatment. This reduces the risk of unwanted tooth movement and improves overall efficiency.
Future Trends in Anchorage Management
What’s next for Anchorage? I think we’ll see even more personalized approaches. Imagine anchorage strategies tailored to each patient’s unique bone structure and treatment goals. Also, research into biological ways to enhance anchorage, like using growth factors to stimulate bone formation around TADs, could be a game-changer.
- More predictable and efficient tooth movement.
- Reduced reliance on patient compliance (no more forgetting to wear headgear!).
- Improved treatment outcomes and shorter treatment times.
Challenges In Anchorage Application
Common Issues with Anchorage Loss
Anchorage loss is a pretty common headache in orthodontics. It happens when the teeth used for anchorage move more than you planned, messing up the whole treatment. Think of it like this: you’re trying to pull one tooth into place, but the tooth you’re using as a ‘fixed point’ starts to budge too. This can extend treatment time and might even mean you don’t get the results you were hoping for.
Here are some things that can cause it:
- Not having enough teeth to act as an anchorage.
- Using too much force.
- Not following the treatment plan closely enough.
- Patient not cooperating (not wearing elastics, for example).
“Early warning signs of knowledge gaps in patient understanding”
Factors Leading to Anchorage Failure
Several things can lead to anchorage failing completely. It’s not just about teeth moving a bit; it’s about the whole system breaking down. Poor planning is a big one. If you don’t accurately assess how much anchorage you’ll need at the start, you’re setting yourself up for trouble. Also, the quality of the bone supporting the anchorage teeth matters. If the bone is weak, those teeth are more likely to shift. Patient compliance is also key. If they aren’t wearing their appliances or following instructions, it can all fall apart. Another factor is the type of malocclusion being treated; some are just inherently more challenging when it comes to anchorage control. Understanding anchorage in orthodontics is crucial for preventing these failures.
Case Studies of Anchorage Challenges
Real-life examples can really show how tricky anchorage can be. Let’s say you’re trying to close a big gap after extracting a tooth. You’re using other teeth as anchorage, but they start to tip forward. Now, not only is the gap not closing as planned, but you’ve also created a new problem with the alignment of the anchorage teeth. Or, imagine a case where a patient has a strong bite force. This extra force can easily overwhelm the anchorage, leading to unwanted tooth movement. These case studies highlight the need for careful planning and monitoring throughout treatment.
Managing anchorage is like balancing a seesaw. You need to carefully consider all the forces at play and make adjustments as needed to keep everything in equilibrium. It’s not always easy, but with good planning and attention to detail, you can minimize the risk of anchorage loss and achieve successful treatment outcomes.
Clinical Implications Of Anchorage
Role of Anchorage in Treatment Outcomes
Anchorage plays a big part in how well orthodontic treatment works out. Without good anchorage, you might not get the tooth movement you’re aiming for, and that can mess up the whole plan. Think of it like building a house; if the foundation isn’t solid, the walls won’t stand straight. In orthodontics, anchorage is your foundation. If you lose anchorage, molars might drift forward when you want to close spaces after extractions, messing up the bite and profile.
Patient-Specific Anchorage Strategies
Not every patient needs the same kind of anchorage. It really depends on their specific situation. Some things to consider:
- How crowded are their teeth?
- What’s their face shape like?
- How strong are their jaw muscles?
“Can interactive tools improve adherence to anchorage-based plans?”
For example, someone with a strong jaw and not much crowding might not need as much anchorage reinforcement as someone with a weaker jaw and a lot of crowding. It’s all about tailoring the approach to the individual. We might use temporary anchorage devices (TADs) for one patient but rely on extraoral headgear for another. It’s a judgment call based on what’s best for them.
Effective anchorage isn’t just about preventing unwanted tooth movement; it’s about creating the right environment for the desired changes to occur. It’s a balance between resisting unwanted forces and allowing the necessary movements to happen efficiently.
Evaluating Anchorage Effectiveness
So, how do you know if your anchorage is working? It’s not always obvious. Here are a few things we look at:
- Are the teeth moving the way we expect them to?
- Are we seeing any unwanted movement in the anchorage teeth?
- Are the patient’s bite and profile improving as planned?
We use X-rays and models to keep track of tooth positions and make sure everything is on track. If we see signs of anchorage loss, we might need to adjust our strategy. This could mean adding more anchorage units, changing the force vectors, or even switching to a different anchorage technique altogether. It’s an ongoing process of monitoring and adjusting to get the best possible outcome.
“Asymptomatic vs symptomatic effects of poor communication”
Wrapping It Up
In conclusion, understanding anchorage in orthodontics is key to effective treatment. It’s all about knowing how to resist unwanted tooth movement while applying the right forces. We’ve looked at different types of anchorage, how they’re classified, and what factors come into play. From the teeth and bone to the muscles involved, each aspect matters. Plus, with advancements in techniques, managing anchorage has become more precise. Whether you’re a patient or a practitioner, grasping these principles can make a big difference in achieving the desired results. So, keep these insights in mind as you navigate the world of orthodontics!
Anchorage Frequently Asked Questions
Question 1. What Is Anchorage In Orthodontics?
Answer: Anchorage is the resistance to unwanted tooth movement during orthodontic treatment. It helps keep certain teeth in place while others are moved.
Question 2. Why Is Anchorage Important In Orthodontic Treatment?
Answer: Anchorage is crucial because it ensures that teeth are moved correctly without causing other teeth to shift in unwanted ways.
Question 3. What Factors Can Affect Anchorage?
Answer: Factors that influence anchorage include the shape and position of teeth, the type of movement needed, and how strong the forces applied are.
Question 4. What Are The Different Types Of Anchorage Techniques?
Answer: There are several types of anchorage techniques, including intraoral methods (using teeth inside the mouth) and extraoral methods (using devices outside the mouth).
Question 5. How Can Orthodontists Prevent Anchorage Loss?
Answer: Orthodontists can prevent anchorage loss by carefully planning treatments, using reinforcement techniques, and controlling the forces applied during treatment.
Question 6. What Are Some Recent Advancements In Anchorage Control?
Answer: Recent advancements include new devices and technology that improve how anchorage is managed, making treatments more effective and efficient.
Leave a Reply