Antimicrobial Drugs General Considerations
Question 1. Write Briefly On Bacterial Resistance To Antimicrobial Agents.
Or
Describe Briefly Drug Resistance.
Or
Explain The Mechanism Of Development Of Bacterial Resistance To Antimicrobial Agents.
Answer:
Drug resistance refers to the tolerance of microorganisms to the inhibitory action of antimicrobials.
“Understanding the role of antimicrobial drugs in treating infections”

“Importance of studying antimicrobial drugs for healthcare professionals”
Types Of Drug Resistance
There are two types of drug resistance, i.e.
- Natural resistance: Various microbes are resistant to certain antibiotics. These bacteria lack metabolic process or the target site which get affected by a particular drug, For Example. Gram-negative bacilli are not affected by penicillin.
- Acquired resistance: This is the resistance that is developed by an organism because of the use of an antimicrobial agent for a long period of time. This type of resistance is a major clinical problem if happens, For Example. Gonococci develop resistant to sulphonamides.
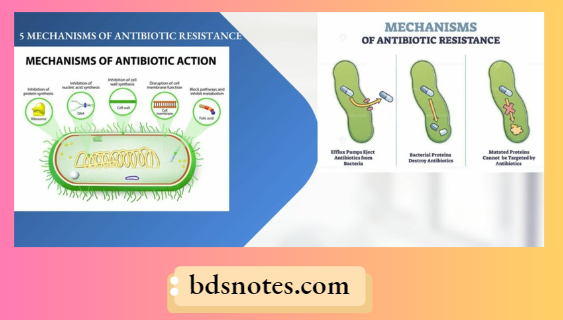
5 Mechanisms Of Antibiotic Resistance
Read And Learn More: Pharmacology Question And Answers
Occurrence Of Drug Resistance
Drug resistance occurs due to mutation or gene transfer.
“Common challenges in managing infections with antimicrobial drugs”
“Role of cell wall disruption in bactericidal drugs”
- Mutation: It’s a genetic change that occurs spontaneously and is not caused by any drug. Any of the sensitive populations of microbes consists of a few mutant cells which require a high concentration of drug for inhibition. These cells are selectively preserved and get the chance to proliferate when sensitive cells are eliminated by the drug. So with time, a sensitive strain is replaced by a resistant strain. Mutation can be a single step or multistep.
- Gene transfer: It is the infection transmitted from one organism to another by conjugation or transduction or transformation.
- Conjugation: It is the sexual contact via the formation of a bridge or sex pilus which is common in Gram-negative bacilli of the same or other species. The gene-carrying resistance or R factor is transferred only if another resistance transfer factor is present.
- Transduction: It is the transfer of gene-carrying resistance via the bacteriophage. R factor is taken up by the phage and delivered to another bacterium that it infects.
- Transformation: A resistant bacterium can release the resistant carrying DNA in a medium and this can be imbibed by another sensitive organism that gets unresponsive to the particular drug.
“Treatment options for infections requiring antimicrobial drugs”
Following are the mechanisms by which a microorganism can develop resistance to an antimicrobial agent.
5 Mechanisms Of Antibiotic Resistance
- Secretion of inactivating enzyme: Microorganisms such as staphylococci, gonococci, etc. secrete β lactamases which destroy penicillin.
- Effl pump mechanism: This prevents the accumulation of drugs in microorganisms, For Example. is the resistance of Gram-positive and Gram-negative bacteria to tetracyclines.
- There is reduced entry of antimicrobial agents in a microorganism because of alteration in the channel which is required for its entry into the microorganism.
- Alteration inside the binding site: Change in penicillin-binding proteins in various pneumococci with a decrease in the affinity for penicillin.
- Absence of metabolic pathway: Bacterias which resist the sulphonamides utilize and perform folic acid without any need for metabolic steps.
“Techniques for managing high-risk groups with infections”
Question 2. Enumerate Drugs Effective In Staphylococcal Infection.
Answer:
The following are the drugs effective in staphylococcal infection:
- Cephalosporins
- Nafcillin or related antibiotics
- Sulfa drugs
- Vancomycin.
Leave a Reply